
适应性支持通气 (ASV) 是一种根据病人的肺力学指标和呼吸用力选择和连续适应呼吸频率、潮气量和吸气时间的通气模式。
按照逐次呼吸,全天候,从插管到拔管。

ASV 自动采用肺保护策略,以最大程度减少内源性 PEEP 和容积伤/气压伤等并发症 (
在肺保护性策略规则下,ASV 可支持病人自主呼吸(

在本视频中,高级医师 Jean-Michel Arnal 博士在真实 ICU 病人中为您快速演示了 ASV 的主要功能和设置。
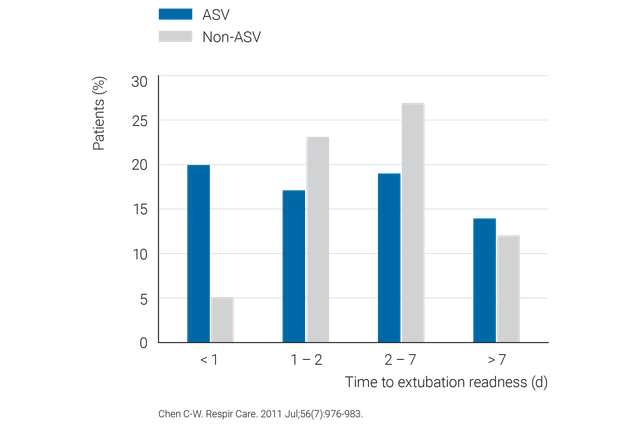

ASV 是我们所有重症监护呼吸机上的一个标准通气模式。